
Four years ago, an incredible scientific discovery went largely unnoticed by mainstream media. A group of American researchers, including some from the University of Massachusetts, managed to “take a photo” of a new life being born, i.e., conception.
It turned out that the emergence of life is accompanied by a flash of light emanating from a spark of inorganic origin, the authors of the groundbreaking study claim in their exhaustive report supplemented by photo and video materials.
The phenomenon, which was named “the zincspark”,gave rise to numerous theological statements to the effect that the mystery of conception is powered by “a spark of God”. Esotericists also picked up the theme of the light of a new life sent from above, and neophilosophers called for “thinking the unthinkable.”
But the purpose of this article is not only to discuss the mystical nature of the mysterious spark, but also to understand how new research will increase the chances of couples or women planning in vitro fertilization to have children. And although the zinc spark remains a little-studied phenomenon, scientists argue that its discovery could make it possible to more accurately determine whether conception has occurred, and significantly reduce the occurrence of unsuccessful in vitro fertilization (IVF).
Now, let’s try to separate beautiful fiction from medical facts, and find out what zinc has to do with all of it.
The phenomenon, which was observed in 2016 by American scientists at Northwestern University under the leadership of Professor Teresa Woodruff, looks mystical. Biologists were able to see a zinc spark, an indicator of successful fertilization and the start of growth of a human embryo. The flashes of light on the monitor, accompanying the fusion of the egg and sperm, were immediately dubbed by many as the “spark of life.” The scientists published the results of their observations in the journal Scientific Reports.
However, the biologists from Teresa Woodruff’s team were only partially pioneers. By their own admission, they received a “generous gift” in the form of an experiment by Dr. Rafael Fissore of the University of Massachusetts Amherst. His laboratory, using experimental mice, investigated and scientifically described the mechanism by which sperm cells start the development of an embryo in an egg. The contact of the sperm with the egg launches a whole cascade of events in the egg: cellular respiration and protein synthesis increase, the flow of ions through the membrane changes, and much more.
One of the key elements of this activation of the egg is its absorption of calcium ions. It was previously known that changes in the concentration of intracellular calcium can predict the state and health of the future embryo. The oocyte activation by calcium ions has been sometimes used to help the in vitro fertilization procedure.
However, a few years ago, scientists noticed that the processes of activation and fertilization of the egg are closely related to the transmembrane flow of other ions as well – those of zinc. In the very first minutes after contact with the sperm, the zygote throws out zinc so actively and quickly that this moment was called “the zinc spark.”
Until now, all such studies have been carried out only on animal cells. The existence of a zinc spark and the role of these ions in the fertilization of a human egg could only be guessed at. Scientists induced the artificial activation of the female ovum by injections of ionomycin and other agents that stimulated the absorption of calcium ions and the release of zinc without contact with the sperm. At the same time, a harmless fluorescent agent was added to the nutrient medium: as it binds to zinc, a bright flash emanates, which the scientists filmed under a microscope.
The researchers figured out the nature of the phenomenon and found that it is zinc atoms that produce sparks; these atoms are emitted by a fertilized egg. It ejects them in waves, one after another, with small interruptions.
Zinc is contained under the shell of the egg in special pockets, of which there are several thousand, and the number of zinc atoms contained in them is about 60 billion. During the “fireworks” 4-5 volleys equaling 10 billion “charges” are launched.
Before the introduction of the sperm, the egg, on the contrary, intensively accumulates zinc, the content of which increases manifold during the period of its maturation. This element helps the cell to mature and develop. But such an amount of zincis unnecessary and even harmful for the embryo; therefore the egg gets rid of it at the time of fertilization.
The most surprising thing: the more intense the glow, the more reliable the result of the transformation of the egg into a full-fledged and healthy embryo.
Scientists admit that they have not revealed the secrets of all the processes that take place during conception. But it is believed that by the intensity of the “fireworks” one can judge the quality of the egg: the brighter it is, the more likely it is that the conception was successful.
This is especially important for artificial insemination procedures – as they say, in a test tube, into which the “spark of life” should also descend.
As of today, there are no reliable methods for predicting the viability of an embryo obtained in this way. Therefore, the final verdict on the future health of the fetus can only be passed after the embryo has been transplanted to a woman.
The implanting of low-quality embryos is the main reason for unsuccessful IVF occurrences. The ability to observe the zinc spark could ensure a successful activation and fertilization of the egg and facilitate the complex IVF procedure.
This is of great practical importance: the fact is that in vitro fertilization is no longer just an achievement of medical science – it has been a part of our life for the last 40 years. On July 25, 2020, the world celebrated the 42nd anniversary of the birth of the first “test tube baby” (Steptoe and Edwards, 1978). Now there are more than 40 million people born as a result of artificial insemination on our planet. The figure is impressive, and, judging by the demand for such medical services, the statistic ispoised for further growth.
Initially an experimental procedure with unpredictable results, IVF quickly developed into a medical service that is highly successful,both clinically and economically. In the United States, in vitro fertilization has largely evolved in private practice outside of academia because Congress excluded it from most government-funded research. Thus, competition between health centers providing these services has contributed to an ever greater success of this alternative to natural conception.
More than 30 years ago, in the mid-1980s, a number of developed states of the United States (e.g., Massachusetts, California, Illinois, Virginia, etc.) introduced various levels of insurance coverage for IVF. Insurance companies in these states began to enter into contracts with clinics, which made the procedure available to many Americans.
Today, almost all states have some level of insurance coverage or special IVF programs. And in 16 out of 50 states, full coverage of the IVF procedure is considered mandatory.
More and more employers in the United States are helping couples with costs in states where IVF coverage is not available. In 2020, big companies like Cisco and MassMutual increased their maternity payments. Starbucks and Chobani even offer IVF coverage to hourly employees. Many tech companies, including Apple, Facebook, and Microsoft, have gone beyond basic IVF payments and cover employees for the cost of freezing and storing embryos.
The European Society for Human Reproduction and Embryology has also compiled data from the national registry of assisted reproductive technology cycles, performed in Europe from 1997 to 2015. Spain was found to lead the continent in assisted reproduction with a record 119,875 treatment cycles. It is followed by Russia (110,723 cycles), Germany (96,512), and the former leader, France (93,918). In the UK, there are typically around 60,000 treatments per year.
In comparison, the US fertility centers in 2016 conducted 263,577 cycles of assisted reproductive technologies to treat infertility, resulting in 76,930 live births.
Today, the United States remains the top in-vitro tourism destination for many Europeans. This is due to several factors:
According to a Business Stats News report, the in vitro fertilization (IVF) market is expected to exceed $ 850 billion by 2026, with an average annual growth rate of 11.1%. According to experts, the demand for in vitro fertilization in the world will grow due to an increase in the level of not only female, but also male infertility. Unfortunately, this is a trend fueled by excessive alcohol consumption, smoking, and environmental pollution. Couples are increasingly resorting to IVF, and, according to 2020 statistics, 12.2 children were born as a result of this procedure for every thousand newborns.
Dr. Maja Barbalić, a molecular biologist and team leader of genom.hr, as well as a co-founder of the startup www.henome.com, states the following:
“It is not always well recognized, but in up to 40% of all cases the reason behind the couple’s infertility lies in a male factor. There are a lot of causes underlying male infertility, and in 30% of cases it is a genetic factor that could be easily detected by genetic testing. This type of testing can even predict the sperm availability in testis that could guide the decision for TESE (testicular sperm extraction), a procedure for sperm retrieval necessary for in vitro fertilization”.
It is also important that in recent decades, there have been social transformations in many countries of the rights of lonely and LGBT people, and laws are being adopted regulating their rights to family and children. It will also increase the number of families who are looking to have children using an in vitro fertilization procedure.
Europe is expected to become the second largest and fastest growing segment of this market.
But there is one complicating factor: as women get older, their chances of pregnancy decrease, says Dr. Elena Yanushpolsky of Brigham and Women’s Hospital in Boston, where the IVF success rate is one of the highest in the world. Dr. Yanushpolsky, who is a recognized authority in the field of reproductive medicine, notes:
“Success rates for artificial pregnancies range from 46% in women under 30 to 13% in those over 40. I can give you some statistics from the Fertility and Reproductive Surgery Center where I work:
– In women under 35 years of age, pregnancy is achieved in 45.6% of cases, and a live birth is achieved in 37.4% of cases.
– The next age group, from 35 to 37 years old, has the corresponding figures of 43% and 35.3%.
– Further, among women from 38 to 40 years old – 33.1% and 23.5%,respectively.
– For those who are 41–42 years old –27% and 14.9%,respectively.
– For women over 42 years old – 11.9% and 7.5%, respectively.”
Since there are still no reliable methods for predicting the “quality” of the embryo, doctors usually introduce them in excess, and this often leads to multiple pregnancies. That is why we have seen so many twins on the streets lately. But not all families are ready for triplets.
For couples undergoing IVF procedure, there is an option of preimplantation testing, PGT, that is used to examine the presence of genetic abnormalities in the embryo.
The PGT test became popular in the 1990s and is still used today as a method to determine the quality of embryos in in-vitro fertilization and to select the most healthy and viable embryo. It is known that the older a woman is, the more likely she is to have chromosomal abnormal embryos. Preimplantation genetic screening (one type of PGT) helps women of all ages increase the chances of a successful pregnancy.
However, the PGT test has one significant drawback. Since its results are based on the analysis of an individual cell, this test does not always realistically assess the state of the whole embryo due to a phenomenon called genetic mosaicism. This is the phenomenon when an organism, has not one but several genetic lines. Genetic mosaicism can result from many different mechanisms that are difficult to foresee.
In addition, the study showed that the results of biopsies of the same embryos in two different laboratories do not always match. And not all women can or should undergo genetic screeningdue to such disadvantages of this technique as the invasiveness of biopsy and the inability to foresee chromosomal mosaicism, which makes the test ineffective.
Alternative methods of determining the quality of an embryo during IVF are microscopy as well as profiling of RNA and protein expression.
*Another important issue is prerequisites and psychological background. Before deciding on IVF, parents-to-be should be prepared for this important step. There are a number of educational courses on this topic, for instance www.fertilityiq.com
The other type of PGT, which is usually referred to as preimplantation diagnosis (PGD), is used to analyze the embryo for specific gene mutations that one or both parents are carrier of and that they can pass down to a child. In PGD, an embryo without those mutations is selected and transferred back to the uterus preventing the occurrence of serious genetic defects in the unborn.
But even if it turns out that embryo carries an unwanted genetic abnormality, the developing CRISPR technology – genetic scissors –might be able to correct the nature. CRISPR technology became a real revolution in medicine, and it seems that soon CRISPR technology will become a “scalpel” preventing many serious hereditary diseases and pathologies.
True, today’s society is not quite ready to use this technology for reproductive purposes, referring it to the eugenics toolkit and a lot of ‘unknowns’ in its implication to the future baby’s health. The full use of CRISRP in the embryo remains taboo: three years ago, a scandal erupted after the embryo gene editing experiment of the Chinese biophysicist He Jiankui that resulted in first babies born with edited genomes. The official authorities imprisoned him by criminalizing the experiment, and the mainstream science condemned He’s actions, saying that gene editing technology was premature for reproductive use.
Twenty years ago, the Hollywood blockbuster Gattaca amazed everyone with its eugenistic plot, but given the dynamics of the development of genetics, it seems that playing with destiny is becoming a reality.
Read our article in Russian.
Like it? Subscribe to our digest www.iLIke.Boston: in it, we highlight what is happening in Boston and Massachusetts, including medicine, bioengineering, and genetics – n the Health & Science section.
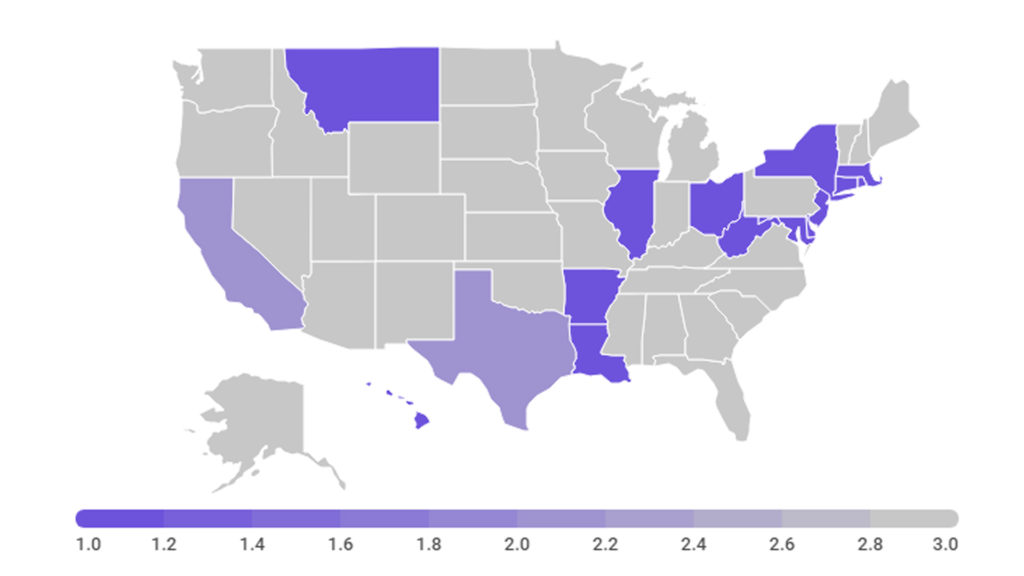
By the way, a little more than a decade ago,an unusual phenomenon was noted in Massachusetts, especially in Boston. It is called another “Mass Miracle”, when the birth of twins or triplets increased to 40 cases per 1000. It happened, at least in part, due to successful IVF procedures, because of which, after multi-implanting, two or more embryos developed. But not only that. A funny statistic took on an epidemic tinge when Massachusetts took the lead in the number of twins, overtaking the African country of Benin, where twin births comprise 28 out of 1,000 births: more than any other country in the world. Find out why it happened, and all about twins,plus how to change two lives.
Write or call us if you are going to Boston, New York, or on a trip to America for business, study, research or a just for a pleasure.